I'd be lying if I said that we weren't having cold feet about the surgery, but I think we know in our hearts that it's the right next step for her. We've written extensively on how we got to this point and what eventually led us to this decision, but if you're just reading this blog for the first time and are looking for the short story, well here it is.
Isabelle was born with several intestinal perforations. She had surgery within the first couple of weeks of her life that created a situation which required her to be intubated for lengthy periods of time and kept her from feeding orally for quite some time. Also, she was born at 1 lb 7 oz and her lower esophageal sphincter (LES) had almost no tone, meaning it wasn't keeping the food down that we were feeding her. We believe that most of this was caused by prematurity and IUGR due to Twin-to-Twin Transfusion Syndrome.
As she healed from the surgery, she was eventually allowed to try to eat by mouth again, but demonstrated some oral aversion and seemed very uncoordinated with her sucking, swallowing, and breathing. She made some improvements while still in the NICU and eventually came home without oxygen, but with an NG tube. She really seemed to struggle with her oral feedings, even though we were receiving input from multiple doctors and therapists on how to potentially treat her eating issues.
Eventually, we came to the conclusion that she needed to be back on oxygen because she was, in essence, trying to run a marathon while eating. She had become so used to it that it didn't bother her, but did affect her eating.
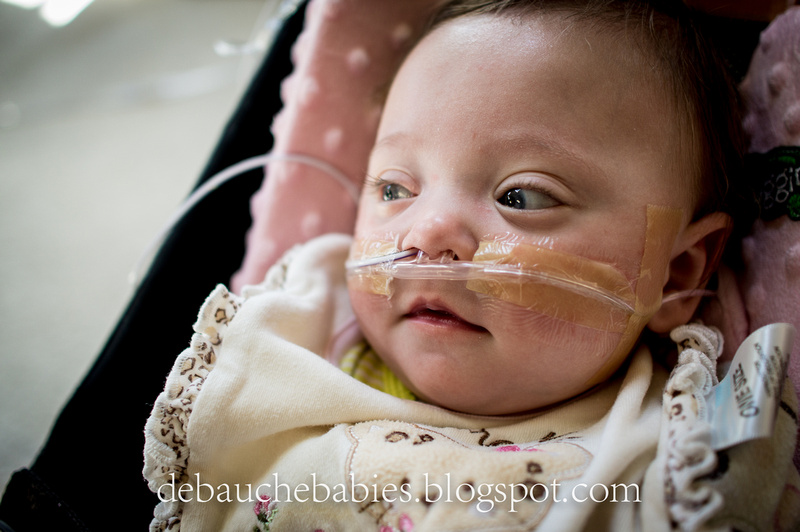
So, for the last couple of months, she's had both the NG tube and the nasal cannula on her face 24 hours a day. On the positive side, she's been gaining weight, good weight. On the negative side, we haven't really been able to increase her daily volume in quite some time, she regularly spits her food up beyond what you would be used to seeing, her reflux is still causing her pain, she spends more than half her day upright either sitting in her bouncy chair or the sitting still in the swing. The latter has resulted in some physical delays that keep her from catching up to her sisters. Essentially, we feel like it's starting to affect her quality of life. If she has it her way, she'll be on the move soon and the last thing we want is for her to be tied down by tubes.
The Nissen will be placed near the LES and will let food down, but not let it back up. We still need a way to feed her when she can't finish her bottle by mouth, as well as the stomach will need a way to vent its gas when the Nissen won't let it come back out. This is where the G tube comes in. So, they kind of go hand-in-hand. Not everyone who gets a G tube needs a Nissen, but logically it makes sense that most who need the Nissen will need a G tube.
I promised the short version, so I'll leave it there.
The surgery isn't supposed to take very long and will be performed by the same surgeon (who we really like) who did her previous bowel surgeries--Dr. Liu. They told us to expect her to stay in the hospital for three to five days. Meg will stay for the weekdays and then I'll swap with her on the weekends so she can see the other girls.
I know that as her parents, we'll never forget these experiences and the sometimes heart-wrenching decisions that accompany them. It's my hope that she grows up not remembering these early painful days and that one day way off in the future, I'll be able to explain to her where her scars came from because she really doesn't remember herself.
Please keep us in your prayers today. We're not expecting anything to go wrong, but it's another surgery and there's always risk, especially when you go under anesthesia.
I'll try to write an update post when we know how the surgery went.
Prayers are being sent your way. I have been a follower of your blog for a long time. I have twin boys born in 2010 at 24 weeks. We had a similar situation with the smaller twin. We opted for the gtube in Feb 2011. We were so scared to get it placed. It was the BEST decision we could have ever made. At first he refused anything by mouth. We had to give him lollipops to try to get him interested in food or liquids by mouth. After many months, he took off, and is now getting his button removed at 18 months old. I know Izzy will take off as well. Reflux is brutal and caused many delays with my son. At 8 months old, he outgrew it, and instantly made up for any delays that he had. It's hard not to compare the development of your other girls to Izzy, I'm sure....but she's fiesty and she will surprise you! I will be thinking of all of you today.
ReplyDeleteBest wishes,
Kerry from Boston
There are many adjectives that describe the girls, sweet, beautiful, playful, amazing. But the one that seems to describe Isabelle best is "resilient". I have watched her have a reflux episode - become diaphoretic, spit up most of the food she just ate, show pain in her eyes when it is happening and then minutes later when all of that has passed you see her sweet wide smile when you call her name and talk to her. She so much loves when you talk to her.
ReplyDeleteMy thoughts and prayers to all of you today.
Love Grandma Jo Anne
Hang in there. I am sure everything will go well for Miss Izzy. Thanks for the update! I'll be thinking of you all today. :)
ReplyDeletePraying for a successful surgery and for the fewest side effects for your sweet girl.
ReplyDeletePrayers for your baby girl to have a successful surgery and a quick recovery and sending lots of strength for mom and dad
ReplyDeleteI just wanted to let you know I am praying for Izzy and your entire family. I am a fellow triplet mom who has followed your posts since the pregnancy. My trio iare 10 months and one of my little guys was born with a heart defect which required open heart surgery at 4 months old. Thankfully surgery was a success and he is thriving and slowly catching up developmentally to his brother and sister. I just wanted to send my prayers and support as someone who not only understands the triplet life but also the added layer of one little one with medical issues. Izzy strikes me as a strong little cookie and you and Meg are great parents!
ReplyDelete